They say, “a horse’s eye is a window to their soul”. That being said, ocular (eye) health for our horses is imperative. We see horses for ocular issues fairly commonly, and any issue with the eye is considered urgent because they can, unfortunately, progress quickly if not addressed.
CORNEAL ULCERATION
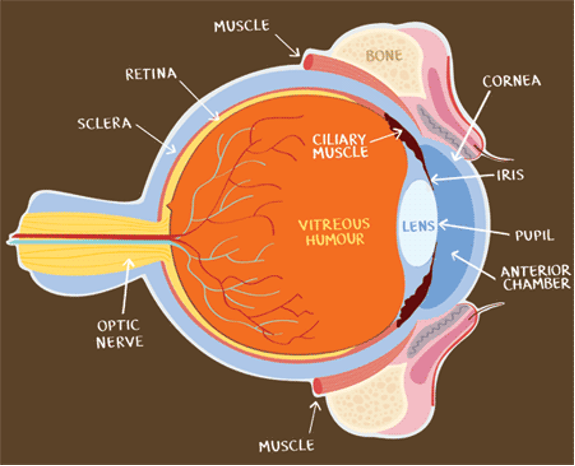
One of the most common ocular conditions we see in the horse is corneal ulcerations. As shown in the image above, the cornea is the outermost layer of the eye. A horse’s cornea is 1-1.5mm thick at the center and 0.8mm at the edges, and it is the only thing protecting the internal structures of the eye from the outside world. Corneal ulceration means that the outer layer (epithelium) of the cornea has become damaged, so the inner layers (endothelium) become exposed. Corneal ulceration can occur for multiple reasons Horses most commonly get them from rubbing their eyes on sticks or fence posts.
Clinical signs of a corneal ulcer include squinting, eye tearing, face rubbing, head shyness.
Corneal ulcers should be treated immediately. If left untreated, they can become infected or damage the corneal layers further and lead to a full corneal perforation (a hole right through the cornea) which is untreatable.
Diagnosis of a corneal ulcer is done with a full ocular exam and fluorescein staining – a stain is applied to the eye, and if the endothelium is exposed, it will take up the stain when examined under a blacklight.
Treatment for a simple corneal ulcer involves topical antibiotics and pain management. Treatment may be altered for deeper ulcers or ulcers with irregular edges. Frequent rechecks are one of the most important factors of ulcer treatment, so any worsening can be caught and addressed as soon as possible.
CONJUNCTIVITIS
Conjunctivitis is inflammation of the conjunctiva, which is the light pink tissue within the eyelids and around the eye itself. Clinical signs of conjunctivitis are redness, swelling, and eye discharge. The causes of conjunctivitis include allergies, irritants, or foreign material in the eye.
Diagnosis of conjunctivitis is made by ruling out other ocular conditions such as corneal ulcerations, and inflammation within the eye.
Treatment for conjunctivitis is typically topical antibiotics +/- topical steroid medication (a corneal ulcer should be ruled out before applying steroids to the eye).
CATARACTS
A cataract is an opacity of the lens. They can be very small (incipient cataract) or affect the entire lens (mature cataract). Cataracts cause blindness, and the larger the cataract is the more severe the blindness is.
Diagnosis of cataracts is done by using ophthalmic lights on the eye to determine if light can pass through the lens or if it is opaque.
Topical anti-inflammatories can help prevent secondary inflammation within the eye due to the cataract. However, the only treatment for cataracts is phacoemulsification surgery, which involves removing the contents from within the lens capsule. This is a very specialized surgery that is only performed by certain ophthalmologists.
EYELID TUMOURS
Squamous cell carcinoma is the most commonly encountered tumour of the horse’s eyelid. It affects the ‘third eyelid’, the small flap of tissue in the inner corner of the eye. The cause is thought to be related to UV light exposure to the tissue and most often occurs in horses with white/pink skin around their eyes. Treatment can involve surgical removal of the third eyelid.
Other tumours that can affect the eyelids are melanoma, most commonly seen in grey horses, as well as sarcoids which are caused by papillomavirus.
EQUINE RECURRENT UVEITIS (ERU) – ‘MOON BLINDNESS’
The uvea is the middle portion of the eye, and uveitis means inflammation of the uvea. ERU is an immune-mediated condition that leads to recurring bouts of uveitis in the eye. Appaloosa’s are the most commonly affected breed. ERU can cause eye pain, tearing, redness, light sensitivity, and the inflammation leads to abnormalities within the eye that can eventually cause blindness. Management of ERU involves control of discomfort and prevention of flare-ups. Most often, topical steroids and/or systemic NSAID medication can be used to control the disease.
Written by Dr. Kristen Wilson
Learn more about Dr. Kristen Wilson here.


